Pregnant women among first without COVID-19 symptoms to be tested in KY. Here’s why.
Julia Bright Crigler was relaxed when she was admitted to the hospital Monday morning in Louisville, expecting that giving birth to her second child might be easier than her first.
She’d been advised the week before to call early that morning and see if any beds were available, and if there were, she should show up, ready to be induced. So, Crigler and her husband arrived at 8 a.m., and she registered, donned her gown and settled into her hospital bed.
While she waited, Crigler was given an opportunity only about 1 percent of Kentuckians have so far had: access to a COVID-19 test, despite her lack of coronavirus symptoms.
For now, Norton Healthcare is able to offer universal testing of expectant moms admitted for delivery, because the hospital acquired 300 rapid testing kits from Cephaid, and just a few days ago, another 300, said Dr. Jennifer Evans, an OBGYN and vice president of Norton Healthcare.
In Kentucky, the new coronavirus has so far spread to more than 4,700 people and killed at least 240. More than 56,500 residents — mostly those with symptoms — have been tested, but that’s quickly increasing. As some non-essential health care offices and businesses begin reopening, more asymptomatic people will be tested out of an abundance of caution. Additional drive-thru COVID-19 testing sites run by Kroger are now giving tests to anyone who wants one. But their capacity, like most, is still limited.
Though Norton was one of the first, other hospitals are poised to deploy their own universal testing methods. Over the next week in Lexington, UK HealthCare, Baptist Health and CHI Saint Joseph will begin universally testing certain groups of patients, including expectant moms admitted for delivery.
As more tests become available, a greater emphasis will be placed on testing swaths of the population without symptoms, since it’ll help medical personnel and state leaders assess how widespread the virus is. That information will be key as Gov. Andy Beshear moves to reopen the economy and reintegrate society.
‘I feel relieved’
Even though Crigler had no symptoms, the stress of pregnancy on the body’s immune system makes her more susceptible to contracting the highly contagious respiratory disease. It’s known that people everywhere catch the virus without ever developing cough, fever or shortness or breath. But one of the big questions researchers and medical professionals are trying to figure out is just how big that group is.
That’s why, two weeks ago, Norton Healthcare starting universally testing all pregnant women admitted for delivery, with a goal of expanding it to other patient groups in the near future, like those admitted for elective surgeries.
“We thought it would be a good idea to test our pregnant moms, that way, we can catch them if they happen to be an asymptomatic carrier, so they don’t take that home and potentially give it to their newborn child,” or the rest of their family, Dr. Evans said.
It’s widely agreed upon in health care: broader coronavirus testing is better. But doing it on a universal scale, meaning testing mostly those without symptoms, is still out of reach for many.
That’s mostly a result of too few supplies: the protective equipment health care staff need to collect samples, and testing kits and materials — each of which is in historically high demand, leaving not enough to go around.
For the most part, Kentucky has only been testing its sickest residents. People over the age of 65 are given priority, and so are frontline health care workers and those with underlying health conditions. That started to change only last week, when Gov. Andy Beshear said anyone who wanted a test could get one at COVID-19 drive-thru testing sites operated by Kroger.
Though the number of tests administered has grown by 82 percent in roughly the last two weeks, overall, it only amounts to a little more than 1 percent of the commonwealth’s population. Per day, the state’s testing rate is less than half of where it needs to be, according to a study from the Harvard Global Health Institute using data from the COVID Tracking Project.
On Wednesday, Beshear said his goal is to administer least 20,000 tests per week, before some social activities start resuming in late May. One of the targeted testing areas is Kentuckians without symptoms: “We’ve got to know how many asymptomatic people there are, and to be able to catch someone who may be asymptomatic and spreading it,” the governor said.
For her sake and for the sake of her soon-to-be-newborn, Crigler wanted to know whether she had the virus, so a nurse stuck a 10-inch-long pliable stick resembling a Q-tip deep into her nose and promptly took the sample to a rapid processing testing machine.
It takes about 45 minutes to an hour to process the results. If Crigler had the virus, health care staff would likely move her to an isolation or negative pressure room to lower the chances of airborne transmission while she gave birth, and recommend separating her from her son, if not in different rooms, then at least six feet apart. She, like the hospital staff around her, would have to wear a mask, and providers caring for her would don more heavy duty personal protective equipment to treat her.
While Crigler waited, she thought about what she would do if her results were positive once she was discharged: Would she wear a mask each time she was around her new son? Should she hold him less? How would she keep her husband and 5-year-old daughter safe? Would she try to regularly disinfect everything she touched, knowing, if she did have it, the chances of her transmitting the virus to her newborn were still high?
After about an hour, the nurse returned with Crigler’s results: they were negative.
“I’m relieved,” she texted from her hospital bed.
Just after 7 p.m., Crigler gave birth to a healthy son and named him Pierce Ryland. The following night in her hospital room, he fell asleep next to her. Out her window, she could see the hospital lit up green — a gesture honoring Kentuckians who’ve died from the virus.
‘Whole new level of scary’
Health care providers understand it’s nerve-wracking for people to visit hospitals during a pandemic. While some reasons for seeking care can be postponed, childbirth obviously can’t, which is why hospitals in Kentucky’s two largest cities have had to adjust in real time how they offer care.
That adjustment includes tempering patient anxieties.
“I am spending a lot of time assuaging fears,” JoAnne Burris, a certified nurse midwife at UK’s Midwife Clinic, said this week.
“Pregnancy and birth is a very special moment that typically is very normal and not related to disease or illness, so when you lay a pandemic over that experience, it understandably adds a layer of anxiety,” she said.
Holli Schulz Friley in Lexington had her own set of fears. That’s why, about three weeks ago, anxious over the outbreak that was rapidly gaining steam in Kentucky, she and her husband wondered whether staying home to give birth to their second child would be safer — a consideration Burris said she’s been vetting more often with patients since the outbreak started.
Ultimately, Friley decided she’d rather be in a hospital “if something went wrong with the baby, or if I hemorrhaged,” she said. “Fear kind of trumped staying home.”
Friley gave birth on April 21 to her daughter, Dolores, at UK Chandler Hospital. Like Crigler, her husband was the only one allowed to visit. She spent the first six hours of her labor at home — something midwives generally recommend, but a decision Friley partially made to minimize her time at the hospital.
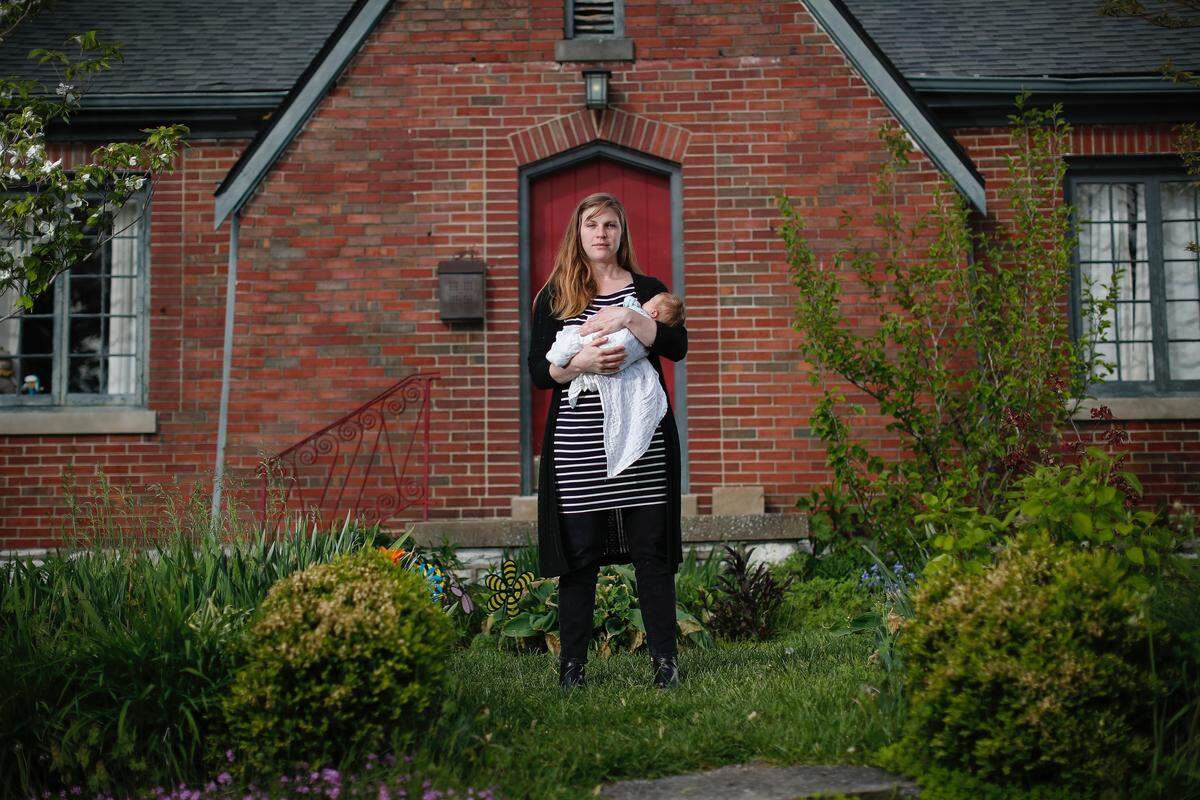
“They pretty much let me know that I should try to labor at home as long as I could,” so that when she finally did get to the hospital, a room would be waiting for her, she said.
The hospital discharged her more promptly for the same reason — typically women admitted for delivery stay a minimum of 48 hours to be monitored. Friley was discharged in about 24.
Dr. John Barton, a perinatologist at Baptist Health Lexington, said, “the goal is to get people in and get people out” as quickly and safely as possible, in order “to limit their exposure to us and our exposure to them.”
Though it’s slated to start next week, UK doesn’t currently offer universal testing for pregnant patients, though patients are screened for coronavirus symptoms upon arrival. Friley, like Crigler, didn’t have symptoms when she went into labor a week ago, but if she’d had the opportunity to get tested, she would’ve wanted to.
“Even just for the piece of mind that I’m not infected and will be starting her off healthy,” Friley said. “It’s already scary anytime a baby gets a fever, but now it’s a whole new level of scary.”
‘A standard of care’
Norton decided on universal testing for OB patients in mid April, around the same time the New England Journal of Medicine published a paper charting COVID-19 infection rates among pregnant patients at a New York City hospital. There, hospital staff tested 215 patients, only four of whom had coronavirus symptoms.
Those four tested positive, but so did 29 other women who showed no symptoms.
In other words, 88 percent of the pregnant patients who tested positive in this study were asymptomatic — a startlingly high rate that caught Evans’ and others’ attention.
Doctors who wrote the paper note the results should be taken with a grain of salt, as not all places have the same rate of cases as New York, an infection hotspot. But their finding “underscores the risk of COVID-19” among pregnant women, they wrote.
“Kentucky thankfully has far lower [infection rates] compared to New York,” Dr. Evans said, but, “If we have that percent [positive] in New York, what does Kentucky look like?”
As of Thursday, close to 300 women have given birth at Norton since universal testing started roughly two weeks ago. Forty-six didn’t want to be tested, but 251 did. Of that tested group, six women without symptoms tested positive.
That amount has surprised Evans — “I thought it may be a little bit higher,” she said. Statewide, about 8.3 percent of those tested have been positive, according to state data.
Burris and other midwives deal with mostly young, healthy women, who, because they don’t have a lot of co-occurring illnesses, “have a good chance of not showing symptoms” if they are infected.
In that case, “we don’t have any reason to know they’re sick, but they’re giving it to people around them,” she said this week.
Without that insight, there’s an inclination to toggle between extremes: to wrongfully assume that everyone is virus free, so no one uses proper personal protective equipment, such as an N95 mask, or the not knowing means staff burn through PPE as a heightened precaution.
“Being able to test everybody who comes in will allow us to direct our care and our precautions appropriately,” Burris said, which helps to conserve PPE.
At Baptist, Dr. Barton has helped set new criteria for how his hospital should care for pregnant patients. He recently co-authored two papers outlining that criteria for the American Journal of Perinatology.
One of those recommendations is for women to limit, if possible, pushing during the final and most grueling stage of labor.
Since the virus is airborne, asking a woman who may or may not be infected to huff and puff even more only increases the chances of exposure to those around her, Barton said.
“If you’ve ever been in a room with somebody pushing for delivery, they’re working hard and breathing hard,” he said. It risks “contaminating a spouse, a support personal, and medical personnel in the room.”
Baptist, like UK, will test patients a few days before their scheduled visits, in order to inform how that patient will be treated, including the type of PPE providers will wear.
Barton expects universal testing to eventually expand to all patient groups, as long as the pandemic is in full swing.
“I can see [testing] becoming a standard of care for hospital admission, until we find something else that’s better,” he said.
Even so, Burris doesn’t want the pandemic to detract completely from the still sacred act of giving birth.
“I have found that birth in a pandemic is equally as sacred and beautiful and safe as it ever was,” she said. While “COVID-19 will be part of a woman’s birth story, it shouldn’t be the story.”
This story was originally published May 1, 2020 at 11:06 AM.
