Half of KY’s public health departments are near bankruptcy. Will this plan save them?
At least once a month, horse and buggies crowd the otherwise vacant gravel parking lot of a satellite Todd County public health clinic.
The buggies are driven by local New Order Amish and Old Order Mennonite families — a demographic that, collectively, totals around 3,000. That’s a fifth of the population in this Western Kentucky county.
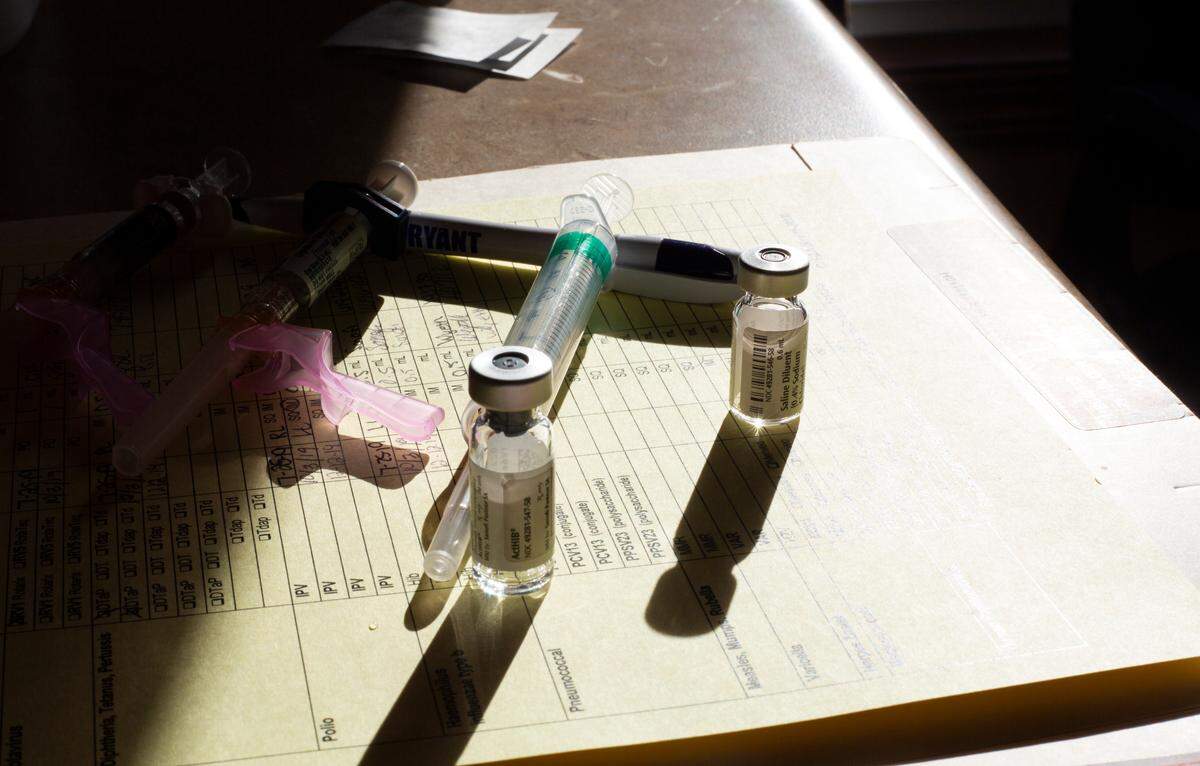
On this mid-December morning, parents carry their bundled infants and lead their toddling children into the waiting room of a small trailer that’s been converted into a clinic specifically for these residents. The children, most of whom only speak Pennsylvania Dutch, are here for vaccinations.
It’s a niche need in Todd County that the public health department, because of strict state and federal funding guidelines, has struggled for years to fund. The fight to pay for these and other services amid exploding pension costs is propelling Todd County and dozens of other health departments across Kentucky toward bankruptcy — a problem that some lawmakers, through a bill this legislative session, believe they can cure.
Cries from pricked little ones echo down the clinic hallway as Norma Jean Horst, 24, removes the bonnet from her 1-year-old daughter, Beverly, who’s due for two shots. A nurse has just given Beverly a red sucker, and she’s clutching it in her small fist.
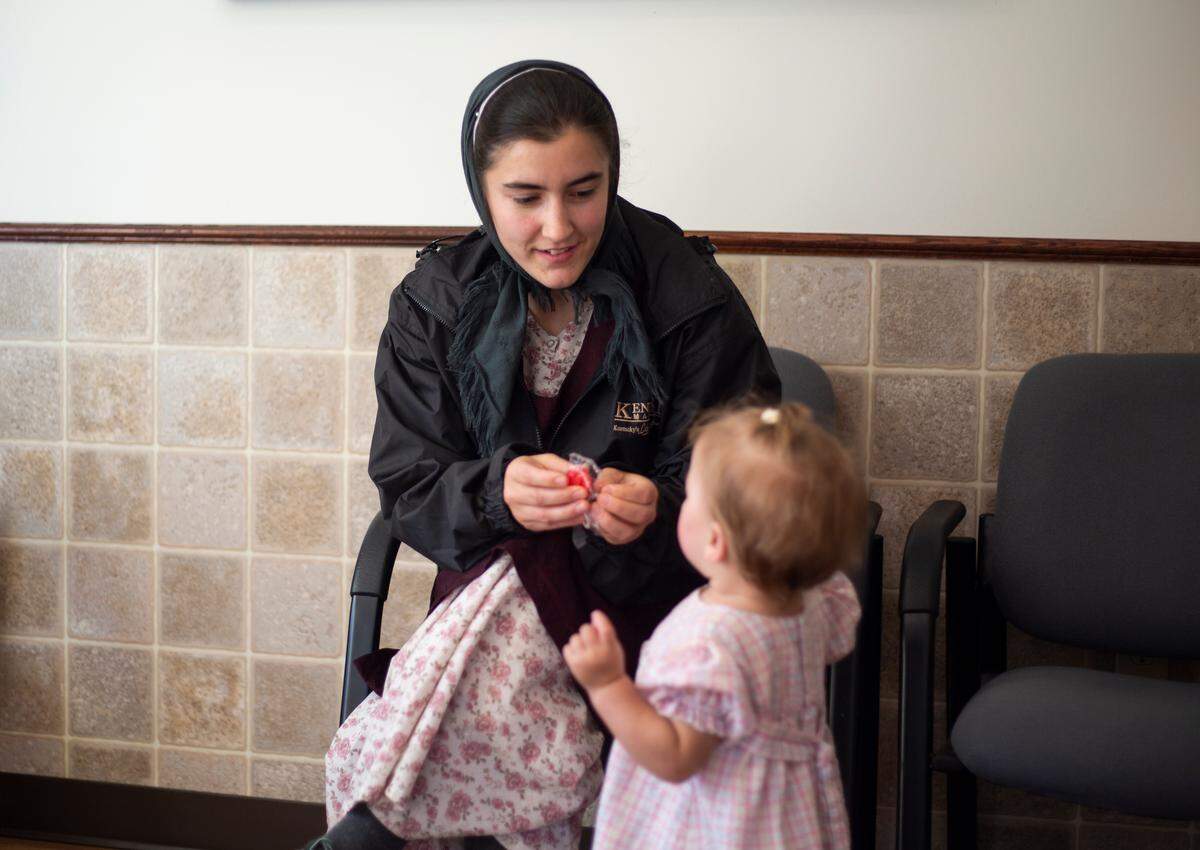
Horst is a Mennonite and lives with her husband and two young daughters about 15 miles away. “It’s really nice for me,” she said of the clinic’s location. “It’s closer for a lot of the Mennonites.” Had it not opened about a year ago, she would’ve traveled, instead, to the flagship Todd County public health clinic in neighboring Elkton, about 10 miles away.
Most practicing Amish and Mennonites in this region, including Horst, don’t have traditional health insurance. Since it’s against their religion to receive Medicaid or other public benefits, they often don’t rely on private providers for health care needs like immunizations.
That’s why, up until a decade ago when Jennifer Harris became director of the Todd County Public Health Department, virtually no Amish or Mennonites in the area were getting vaccinated, she remembers.
Considering the potential impact wrought on the wider county population should there be an outbreak of Measles or Pertussis, Harris decided immunizing them was a clear public health need.
So, in 2010 she started the county’s first Amish- and Mennonite-centric vaccination clinic in the corner of Dutch Kuntry, a local Amish-run grocery store and deli in nearby Pembroke. Momentum built through the years, and it eventually grew to occupy the Fairview clinic. It’s a smaller version of a program the department administers, on its own dime, in the county’s public school system, which has vaccinated nearly 2,000 students in the last two years. Since 2018, 930 Amish and Mennonite children have received immunizations through Harris’ department, at a cost of about $5,000 a year.

“Some people will say, ‘How is that public health?’,” since the clinic is only directly serving a small portion of the greater population, Harris said in her office later that day. “But getting these kids vaccinated is protecting everyone. If you have a fifth of your population who isn’t vaccinated, then your whole public is at risk. That’s how we have to think about it.”
That reality, though, is largely ignored by strict rules that guide how the state funds its more than 60 public health departments.
State and federal funding guidelines have, for years, blocked departments from investing in local priorities if they don’t match the state’s, more than half a dozen public health officials interviewed for this story said.
“Public health shouldn’t look like it does here in Todd County in McCreary County,” Harris said. “We have different people who have different needs. You can’t pin us into silos and expect health outcomes to get better.”
Todd County Public Health receives roughly $92,000 each year in state and federal money to offer the minimum statutorily-required services, such as restaurant inspections, communicable disease investigations, responding to nuisance complaints, and sexually-transmitted disease testing. But the actual cost of these services is closer to $342,000, Harris said.
Additional priorities Harris has pinpointed, like this Amish and Mennonite clinic, are not mandated, meaning state and federal dollars cannot be used to pay for them.

This funding gap has forced Harris into a tenuous position: cobble together additional money through grants and property taxes to continue offering services deemed by her but not the state as imperative, or opt only to fund state-mandated programs.
Like many public health directors across Kentucky familiar with this dilemma, Harris chose both.
The total cost to run her department is $1.6 million — about $813,000 of which is not supported by state and federal dollars. A local option public health tax helps fill the gap, but since it’s based on property values, each community’s ability to contribute can vary widely.
This differential is not unique to Todd County. A majority of Kentucky’s public health departments have been left severely strapped for cash by flat reimbursement rates for the uninsured and Medicaid patients in the face of rising cost of services; state- and federally-mandated program requirements that force many departments to burn resources by duplicating services with other area providers; skyrocketing pension obligations; and a discrepancy between money the state earmarks for certain programs versus the actual, higher cost of administering those programs.
It’s a broken system, Harris said, one that’s “governed by disparate, voluminous and outdated” laws, senior Department for Public Health officials told a panel of lawmakers in a September legislative committee meeting.
Pension woes
Last year’s state pension overhaul, championed by former Republican Gov. Matt Bevin, was the straw that broke the camel’s back. Years of inadequate pension contributions have left the state with $30 billion in debt for the state’s two financially-ailing pension systems, requiring Kentucky to contribute $2 billion each year.
It costs about $106 million for all of Kentucky health departments to offer baseline statutory services — about a third of the actual operational cost — and state money for local foundational services only covers about $27 million, 75 percent of which now goes into the state retirement system.
“When I started here in 2010, our pension cost was about 11 percent of each person’s salary,” Harris said. “This year, it’s going to be 93 percent. When you have that kind of an increase, along with some of our funding going away, it’s just a snowball effect.”

Now, more than half of the commonwealth’s health departments are racing toward imminent bankruptcy. By the end of the 2020 fiscal year, health departments across 41 counties — including Todd County — are projected to become financially insolvent. By the end of 2021, another 22 will be, according to state data. Most of those acutely affected are in rural and Eastern Kentucky. The collective budget shortfall is nearly $40 million.
In order to regain financial stability and offset pension contributions, Gov. Andy Beshear’s biennial spending plan, unveiled last week, proposes spending $33 million to help offset the rising pension costs of public health departments over the next two years.
Prior to this announcement, lawmakers, with heavy input from health directors like Harris, proposed their own historic overhaul of the state’s public health network in the form of bipartisan emergency legislation, known as the Public Health Transformation Plan.
The bill includes a $13.7 million request to the state to help departments get back on their feet, on top of the $27 million the state already invests, state Rep. Kimberly Moser, R-Taylor Mill, the bill’s lead sponsor, told the House Committee on Health, Welfare and Family Services last month.
It also proposes altering the state’s funding formula to a more equitable model — one that would give more money to departments who have little ability to adequately fill funding gaps with property taxes. Larger, more urban departments, such as Fayette County, would likely get significantly less state aid.
The new law would also enshrine local autonomy in state statute, granting public health departments the power, for the first time, to refuse otherwise uniform state programmatic funding they don’t need in order to invest in services they do.
Without passage of this bill in Todd County, the Amish and Mennonite and public school vaccination clinics would be some of the first services cleaved from the budget, because Harris can no longer afford them.
In her office earlier this month, Dr. Angela Dearinger, former commissioner for the state Department for Public Health, said this overhaul and the state’s financial investment is crucial.
“We have poor health rankings [and] our health departments are about to go bankrupt,” she said. “We need a radical approach.”
‘Opportunity to choose health’
Only once since 1990 has Kentucky risen out its rank as one of the 10 least healthy states, according to America’s Health Rankings.
Today, Kentucky ranks 49th in health outcomes. Residents’ high rate of smoking — 49th in nation — coupled with inactivity — 50th — contribute to some of the highest levels of child and adult obesity, heart disease, diabetes and cancer.
Kentucky is categorically one of the unhealthiest states in the country, but its investment in public health is disproportionately shallow, at $87 per person — 27th, overall. The Bluegrass barely outspent the $86 per person Connecticutians invested in public health last year, when their state ranked fourth healthiest.
Allison Adams, director of the Buffalo Trace District Health Department, thinks this disparity, alone, is reason to transform Kentucky’s ailing system. Not only do departments need a greater buy-in from the state, Kentuckians’ understanding of public health needs redefining.
“We tend to think health equals health care or health access, and it doesn’t,” Adams, who’s one of the bill architects and president of the Kentucky Public Health Association, said in her Maysville office. “Ten percent of a person’s health is made up of their ability to access health care. Who’s taking care of the other 90 percent, helping them to choose healthy behaviors? Who’s caring that they have a walkable community?”
The way to do that, she said, is “you move further upstream in the prevention, so you’re changing the opportunity to choose health.”
Take a public health department’s role to prevent teenage pregnancy, for example. Historically, Adam’s likely wouldn’t go beyond ensuring contraceptives were available and that nurses were on staff to administer them.
But paying for these services and so many others using state and federal dollars comes with “deliverables,” or the expectation of how money will be spent. Often, there’s not enough money to reach the mandated goal.
Adams tells it like this: “If I give you $10 to go to the grocery store to get these 10 items, but you get there and the items cost $15, I still expect you to get those things with your $10,” she said. That means to meet that mark, “you have to spend your own $5,” which, in this case, would come from local public health tax dollars.
Today, she receives no federal family planning money, in large part because too few people used her department for those specific in-house services to warrant the traditional investment. Instead, under the transformation model, which Adams slowly began adopting in 2011, she uses local tax dollars to coordinate with local schools to develop curriculum and outreach programs that teach young people self-worth and self-efficacy so that, down the road, they’re more likely to have safe and responsible sex.
Those women who do need family planning services are referred to another area provider, who can provide comprehensive care, Adams said.
This transferring of services is another tenet of public health transformation, but it’s controversial because it counteracts how public health has been historically administered, she said.
In its 2020-2022 preview of the state’s budget, the Kentucky Center for Economic Policy referred to this proposal as an attempt to “scale back the services offered by local public health departments to the bare statutory minimum with the goal of offloading those responsibilities to local private providers.”
Adams called this a “skewed perspective.”
“We do a disservice to folks who come into our clinic for just one prevention service if there’s a community partner out there who can give them comprehensive medical care,” she said.
For example, breast and cervical cancer screenings used to be a mandated service offered by public health departments that comes with a lot of deliverables. Accepting that money means a department must hire nurses who can perform those screenings, even if it’s not an active patient need.
In Adams’ department, it meant, hiring nursing staff because “I had to be ready for a woman in need of a breast and cervical exam, because I was expected to deliver it,” she said. “But we can’t keep throwing away money, waiting for people to walk through the public health department door” for these types of clinical services. Because, she said, “they’re not.”
‘What it should be’
“Most people are misinformed about what public health actually is,” said Georgia Heise, director of the Three Rivers District Health Department, which spans Carroll, Gallatin, Owen and Pendleton counties.
It’s “what we do as a society, collectively, to ensure the conditions for which all people can be healthy,” she said. That can include walkable communities, steady employment rates, access to healthy food, policies and infrastructure that encourage healthy choices, and affordable health care.
Heise’s take is on par with Kentucky’s still-standing definition from 1954: the state is charged to “adequately safeguard the health of all its citizens” by implementing and maintaining “appropriate services for the purpose of protecting the public health” of residents.
But somewhere along the way, public health veered into primarily clinical services. In 2000, when Heise got her first job in Kentucky’s system, she said, “it was clear to me right away that it was not what it should be.”
Today, it’s still a system that rewards treating a problem “one individual at a time,” she said.
But research shows investment in the wider public health system brings worthwhile results.
Between 1993 and 2005, a $10-per-capita increase in local public health spending led to a more than 7 percent decrease in infectious disease rates and morbidity, according to a 2012 study in the Public Health Reports journal.
A 2018 study in Academy Health concluded that evidence is “nearly unanimous that higher total public health spending is tied to better health outcomes.”
Under the proposed bill, Harris’ department is projected to get an additional $52,000; Adams’ district , an estimated $224,000; and Heise’s, $291,000. But even in parts of the state that are projected to lose state assistance, most public health directors favor the proposal.
The Lexington-Fayette County Public Health Department, for example, would lose about $746,000.
But department Commissioner Kraig Humbaugh said he supports the measure in spite of his department’s expected losses.
“We have to be mindful that if other health departments close their doors, that could result in an impact on us,” he said. “It’s time for us to look at what’s best for the entire public health system in Kentucky.”
This story was originally published February 3, 2020 at 10:27 AM.
