‘It is miserable.’ Inmates battling opioid use are often left without help. Why it harms KY
READ MORE
How Kentucky is addressing the opioid epidemic
Expand All

‘It is miserable.’ Inmates battling opioid use are often left without help. Why it harms KY

‘Kentucky shouldn’t wait.’ What the state is doing to address the opioid epidemic
High rate of KY inmates face drug charges. Do jailers see better way to handle drug use?

‘It’s a human right.’ Inmates should have access to opioid withdrawal medications, advocate says
When Erin Cox was jailed at a Central Kentucky detention center in 2018, she was denied access to medicine she’d just begun using to recover from opioid use disorder — the rejection of her medicine sent her into withdrawal.
Still suffering from substance use and without access to medicine she’d been prescribed, she suffered acute withdrawal symptoms — including insomnia, vomiting, shaking and sweating.
“They don’t provide you with anything to help with that withdrawal,” Cox said. “You have to buy that yourself with a commissary and not everyone has access to commissary. When I was in there I was honest with them and told them I was on Suboxone, and I remember the nurse telling me that, ‘I shouldn’t have been on that for more than two weeks.’ I was really offended by that.
“It is miserable because when you are going through withdrawal you have that insomnia. And you already can’t sleep in jail and rest and that makes it even worse. Your body aches and it is like your bones hurt. You can’t get comfortable. You toss and turn. You are sleeping on a thin mat on top of a big slab of steel tossing and turning.”
The issues Cox faced are not uncommon in Kentucky. Only a select number of local jails in the state offer access to select medications for opioid use disorder, leaving many like Cox to be denied treatment and heightening their chance of going into relapse.
This could ultimately lead to greater mortality, as national studies show that within the first two weeks after release, the risk of death from drug overdose is 12.7 times higher than the general population.
Cox left jail and was able to get back on Suboxone – a partial opioid agonist which blocks receptors in the brain that crave opioids, without activating the receptors to create a “high.” She has been sober since 2018 and works as a recovery coach with Voices of Hope.
“When I got out, I was looking for a way to feel better instantly, and thank gosh I was able to find Suboxone and not turn back to the opioids,” she said. “But some people, when they come out, and they are already going through all of that, you know, they are going to turn to the first thing they can find to give them some kind of relief.”
How treating opioid use can reduce ‘societal burdens’
Forced withdrawal during incarceration can push others back into substance use. Cox, policy strategists, lawmakers, members of the recovery community and health care providers are hoping to change the stigma surrounding substance use disorder and medication for opioid use disorder.
“It is already hard being incarcerated and having to do that, but to go in there and withdraw from anything makes it 10 times worse,” Cox said. “Access to human medication like that – it’s a human right. If you are already on the medication, you should be able to still have access to that medication when you are incarcerated.”
An estimated 85% of U.S. prisoners have an active substance use disorder, yet a small portion of those inmates receive clinical treatment, according to the National Institute on Drug Abuse. Health care providers say opioid agonist maintenance is among the most effective treatments for opioid use disorder and maintenance treatment reduces illicit opioid use, crime, recidivism and costs.
But few correctional facilities provide this treatment.
“Decades of science shows that providing comprehensive substance use treatment to criminal offenders while incarcerated works, reducing both drug use and crime after an inmate returns to the community,” a June 2020 report from the National Institute on Drug Abuse said.
“Treatment while in jail or prison is critical to reducing overall crime and other drug-related societal burdens — such as lost job productivity, family disintegration and recidivism. Inadequate treatment while incarcerated also contributes to overdoses and deaths when inmates leave the prison system.”
Dr. Laura Fanucchi, a professor at the Center on Drug and Alcohol Research at the University of Kentucky, said that treatments like buprenorphine and methadone reduce the risk of death from opioid use disorder by more than 50%, making it a highly effective treatment.
“The problem is that far fewer people receive that treatment than would be eligible for it,” she said. “So population wise, there are estimates across the U.S. that we give medications for (opioid use disorder) to fewer than 10% of the people that could potentially benefit from it.”
The National Academy of Sciences reports that number is even lower, with only 5% of people suffering from opioid use disorder in jail and prison settings receiving medication.
Fanucchi said of the patients they see in the hospital, about 75% accept treatment with medication.
“It is much higher than the 10% seen nationwide. We are making progress but there is a lot to be done still,” she said.
Not only would further access to medication and substance use treatment reap benefits to millions of people it affects, but reports indicate it would reduce the overall cost to society.
A report from the National Drug Intelligence Center estimated that the cost to society for drug use was $193 billion in 2007. Of that, $113 billion was associated with drug related crime, including criminal justice system costs and costs borne by victims of crime.
The same report showed the cost of treating drug use (including health costs, hospitalizations and government specialty treatment) was estimated to be $14.6 billion.
Where can inmates get medicine for substance use?
The Kentucky Department of Corrections offers a pilot program called Supportive Assistance with Medication Addiction Treatment which provides certain medications – naltrexone (Vivitrol®) and oral buprenorphine (Suboxone®) followed by buprenorphine (Sublocade®) – at all 14 state institutions as well as 18 local jails.
In 2015, the Kentucky General Assembly passed a law to provide $3 million to the state corrections department to provide medication for addiction treatment in conjunction with evidence-based substance use disorder treatment, utilizing naltrexone prior to release from incarceration, according to the Kentucky Department of Corrections.
The medication treatment program started in 2016 and was expanded in 2018 to the contracted jails that offer the substance abuse treatment program overseen by the Kentucky Department of Corrections.
In 2019, the Department of Corrections received a grant through the Kentucky Opioid Response Effort to expand medication for substance use disorder.
The grant was intended to include utilizing buprenorphine at select pilot locations, including the Kentucky Correctional Institution for Women, the Northpoint Training Center and the Blackburn Correctional Complex.
Due to the extensive federal regulations regarding the use of methadone, the limited funding was used to implement buprenorphine, according to Katherine Williams, communications manager for the Department of Corrections. The supportive treatment program is for individuals within 60 days of release, Williams said.
“In addition to the SAMAT program, the DOC is also providing medical and clinical assessments at intake if someone is on a medication to determine if continuation of medication is appropriate,” she said in an emailed statement to the Herald-Leader. “If so, the individual will be allowed to continue that medication.
“DOC staff are assigned to assist with continuity of care and connections for community providers for continued treatment.”
As of December 2022, the corrections department had 101 state inmates in Kentucky prisons receiving treatment, according to Williams. According to the Prison Policy Initiative, there are 24,000 people housed in state prisons. The number of inmates participating at local jails was not provided.
A report published in April 2022 evaluating the pilot program revealed that more than 50% of individuals involved in the pilot study were still receiving medication for opioid use six months after their incarceration.
“These results indicate that participants continue to engage in treatment post-release, and that linkages with systems of care and support have been successful,” the report said.
The study also showed substance use significantly lowered. At the beginning of treatment study, 81% of participants reported using opioids during the 30 days prior to incarceration — primarily prescription opioids and heroin. At a six month follow up, only one participant reported use of opioids in the previous 30 days, and none reported experiencing an overdose in the past six months.
‘That choice is taken away from them.’
With limited access to medication for opioid use disorder in certain jails throughout the state, health care providers and some in the recovery community say what is offered right now is not enough. But before medication use can be expanded, they believe people need to break the stigma around substance use disorder.
“People with diabetes have to take insulin everyday or other medications and people with heart disease have to take medication everyday because it is a preventative measure,” said Cox. “Same thing with medication – it is a preventative measure. It is just a tool to help you in your recovery. Some people need it short term and some people need it long term.
“That is for them to decide and that is ok. That should be accepted.”
Like Cox and Fanucchi, Dr. Anna Maria South said opioid use disorder is like any other chronic medical disease affecting the brain. South is an associate professor at UK and an addiction medicine physician.
“I think the biggest thing we need to tackle is that people think it is a choice, but it is a chronic medical disease,” South said. “I think if you treat addiction like a chronic medical disease that we have treatment for, that we have life-saving treatment for, then everything falls into place. No other medical disease do we withhold medications for when people get incarcerated.”
She said efforts to punish people with substance use disorders — forcing them to white knuckle through withdrawal — contributes to the stigma.
“It is still the patient’s choice to decline the medication, just like everyone that is not incarcerated has the choice to not receive medication,” South said. “But when people get incarcerated here in Kentucky, that choice is taken away from them. That is wrong. Ethically wrong, medically wrong and it leads to people dying.”
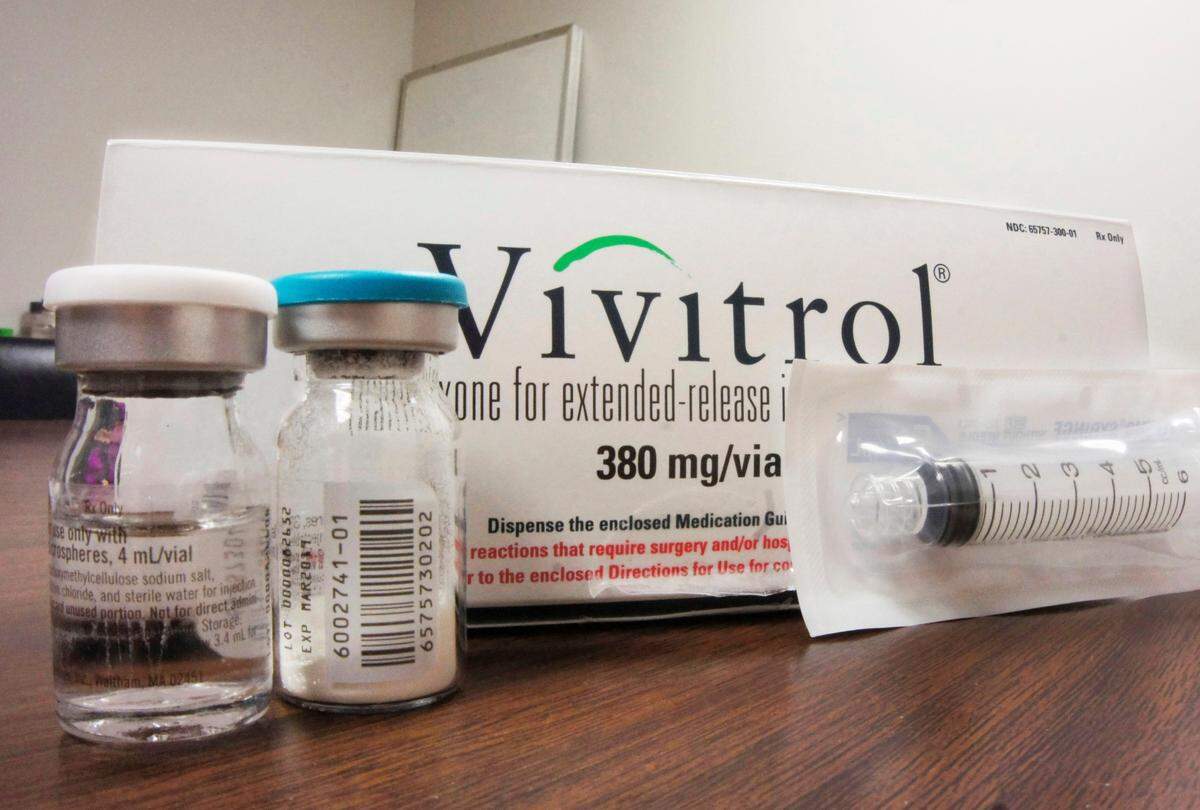
South said in most cases, jails and prisons provide Vivitrol, a long-acting injectable medication which has no data to prove it reduces mortality. However, some places had used the medication to taper inmates off of their original treatment plans including methadone or Suboxone.
“If someone has (type 1) diabetes, and is insulin-dependent and they taper them off their insulin, but offer them something like metformin instead – that wouldn’t work for this patient,” South explained. “That patient would go into (diabetic ketoacidosis) and die.
“For me this is just ludicrous to know that you have someone who is potentially stable on bupenorphine or methadone, has a chronic medical disease, gets incarcerated and has a medical disease that gets destabilized not by an individualized medical assessment that says, ‘You no longer need methadone,’ but that, ‘This is our policy.’ This to me is mind blowing because this does not happen with any other medical disease.”
South said addiction is a chronic medical disease and withholding medication for it “is the biggest stigma.”
This story was originally published January 26, 2023 at 10:00 AM.
